Bunion
Introduction
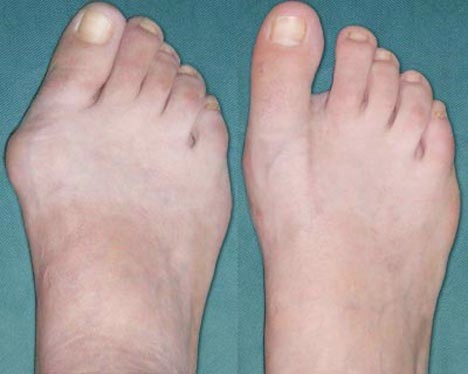 If the joint that connects your big toe to your foot has a swollen, sore bump, you may have a bunion. More than half of women in the UK have bunions, a common deformity often due to wearing tight, narrow shoes, and high heels. Nine out of ten women wear shoes that are too small. Too-tight shoes can also cause other disabling foot problems like corns, calluses and hammertoes.
If the joint that connects your big toe to your foot has a swollen, sore bump, you may have a bunion. More than half of women in the UK have bunions, a common deformity often due to wearing tight, narrow shoes, and high heels. Nine out of ten women wear shoes that are too small. Too-tight shoes can also cause other disabling foot problems like corns, calluses and hammertoes.
With a bunion, the base of your big toe (metatarsophalangeal joint) gets larger and sticks out. The skin over it may be red and tender. Wearing any type of shoe may be painful. This joint flexes with every step you take. The bigger your bunion gets, the more it hurts to walk. Your big toe may angle toward your second toe, or even cross over or under it. The skin on the bottom of your foot may become thicker and painful. Pressure from your big toe may force your second toe out of alignment, sometimes overlapping your third toe. If your bunion gets too severe, it may be difficult to walk. Your pain may become chronic and you may develop arthritis.
Conservative (non-operative) management
Most bunions are treatable without surgery.
Prevention is always best. To minimize your chances of developing a bunion, never force your foot into a shoe that doesn't fit. Choose shoes that conform to the shape of your feet. Go for shoes with wide insteps, broad toes and soft soles. Avoid shoes that are short, tight or sharply pointed, and those with heels higher than 2 1/4 inches.
Treatment options, if you already have a bunion, you should wear shoes that are roomy enough to not put pressure on it. This should relieve most of your pain. You may want to have your shoes stretched out professionally. You may also try protective pads to cushion the painful area.
If you are flat-footed then arch supports and calf stretching exercises may be appropriate.
Surgery
If your bunion has progressed to the point where you have difficulty walking, or experience pain despite accomodative shoes, you may need surgery. Bunion surgery is not simple surgery. The objective is to realign the big toe bones and joint so your big toe can be brought back to a straighter position. Orthopaedic surgeons have several operative techniques and usually they are done as a daycase. However, a long recovery is common and problems may occur including persistent swelling, discomfort and stiffness.
Indications
A Scarf osteotomy is a type of procedure for hallux valgus and the term “scarf” describes the shape of the bone cut (osteotomy) that the surgeon uses. It was popularized in Europe and the term originates from an architectural and carpentry term defined as: “a joint made by notching, grooving, or otherwise cutting the ends of two pieces and fastening them together so that they lap over and join firmly into one continuous piece.”
Operative Procedure
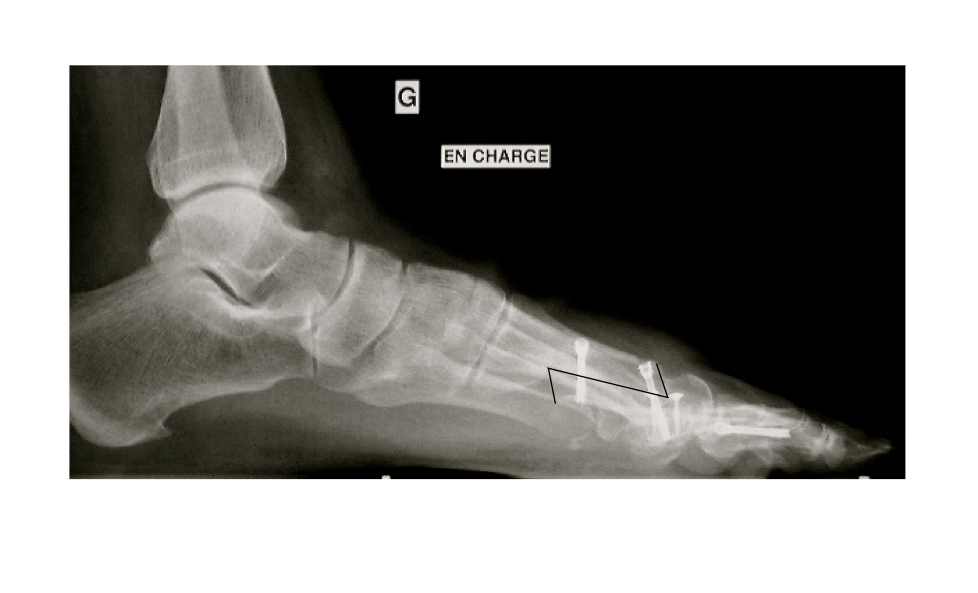
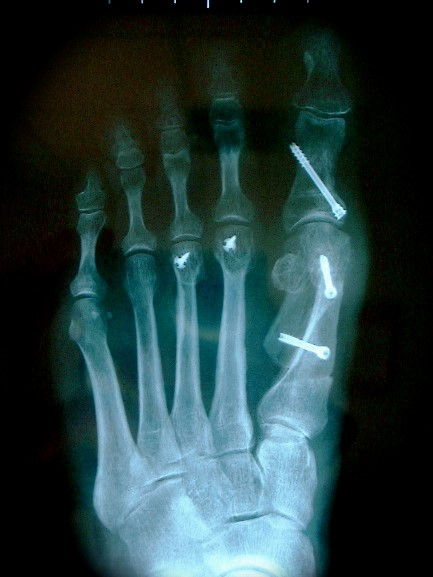
The osteotomy in itself involves a Z-shaped cut in the first metatarsal which can then be moved and fixed in this new position, usually with two small screws. The excess bone on the inside of the foot (medial side) is then removed. The procedure to correct hallux valgus also involves a release of the tight ligaments (lateral release) and tightening of the loose ligaments (medial plication) to balance the joint. Often another osteotomy called an Akin is made in the proximal phalanx (first bone of the great toe) to complete the surgical correction.
The foot is usually then supported in a bandage and the patient can weight-bear more from the heel for up to 6 weeks.
There are risks and complications with all operations and these should be discussed in detail with your specialist. However, with bunion surgery it is important to remember that you may be left with some pain and stiffness and the deformity may reoccur in the future. This is why it is not advisable to have surgery if the deformity is not causing significant pain and does not limit your walking or normal activities.
Although every effort is made to reduce complications, these can still occur. In addition to the general complications that can occur with foot surgery, there are some.
Specific risks with bunion surgery:
- The toe may not be perfectly straight.
- The toe may be stiffer than before the operation, which could affect the heel height of the shoes you wear. Whilst this may improve it can be permanent.
- You may get discomfort in other parts of your foot during the recovery period. This generally settles.
- A small number of patients get overloading beneath the ball of the foot / small toes due to reduced function of the big toe joint. This is known as transfer pain or metatarsalgia. If this is permanent, special insoles or further surgery may be recommended
- There is always a possibility that the deformity may return in later life
General Complications
Pain / swelling
All surgery results in a degree of pain and swelling, generally dependent upon the type of operation. Swelling causes discomfort and, following foot surgery, this can be reduced by keeping the foot and leg elevated level with your heart. Too much activity in the early post operative period can increase the amount of swelling. Following the post operative instructions specific for the operation will help to minimise this complication.
Infection
There is a small risk of infection which is generally superficial, around the wound. If this occurs, this is usually managed successfully with antibiotics.
However, it can be deeper and involve the bone (osteomyelitis). This is infrequent with foot surgery but is a serious complication if it occurs. It often requires treatment with intravenous antibiotics, requiring a stay in hospital, followed by a long period of oral (tablets) antibiotics. In some cases, surgical removal of the bone is required and this can leave the foot less functional.
Although very uncommon, foot infections can be fatal as can any infection. Early recognition and treatment is essential to reduce the risk of serious complication.
Deep vein Thrombosis (DVT)
Due to the relative immobility following foot surgery, there is a risk of DVT much like there is a risk when flying. Fortunately, this is infrequent and appropriate exercises during the post operative period can reduce the risk. Certain operations, requiring plaster cast immobilisation can increase this risk. Preventative treatments are available if a patient has a known risk.
Delayed healing
Although information is provided regarding the likely healing time following surgery, this does vary between individuals. There is always a risk that it may take longer. This could either be the skin (soft tissue) or bone.
Delayed bone healing can take several months to settle and in some cases, it does not heal properly. This is termed a non union and can occur with any bone operation but is more common in some than others. Cessation of smoking reduces the risk. If non union occurs, it is not always painful. However, if it is causing a problem, further surgery may be required. This usually involves removing the area of non healing bone and replacing it with healthy bone from another site (bone grafting). This obviously prolongs the healing time considerably.
Scarring
All operations result in a scar. Whilst the vast majority settle, some can take longer to heal. It is possible that it will be painful, have some nerve entrapment, be discoloured and may become thickened. Whilst every care is taken during the operation, problems can occur. Fortunately, they are usually short term but can be long term. Certain skin types (e.g. Afro-Caribbean) are more predisposed to thickened scars known as keloid scars.
Chronic regional pain syndrome
Previously called reflex sympathetic dystrophy, this is an extremely uncommon condition that can occur following injury (including surgery). The exact process is not fully understood but, essentially, the body over reacts to the injury and becomes extremely sensitive and painful. Even the lightest touch or movement can be unbearable and this can be disabling. Treatment is required by a specialist pain clinic and successful treatment is significantly improved by an early diagnosis (within 6 months).
Recurrence
Despite the best planning and surgery, studies evaluating the outcomes of foot surgery all indicate that problems can re-occur. Whilst every effort is taken to ensure a successful long term outcome this cannot be guaranteed.
Hallux Varus
This result from overcorrection of the bunion deformity. In this deformity the toe start to point inwards. This may affect while wearing closed toe box shoe. Treatment for this will be conservative using straps to align with the other toes. Surgery is reserved for advanced deformity, will be by realignment of the toe or by permanaent stiffening of the MTP joint(Fusion).
Continued shoe difficulty
The nature of foot surgery is such that, even if the underlying problem is resolved / corrected, there may still be residual discomfort or prolonged swelling. As a result, there could be continued difficulty with shoes. Women often wish to return to fashionable shoes and this can by no means be guaranteed.